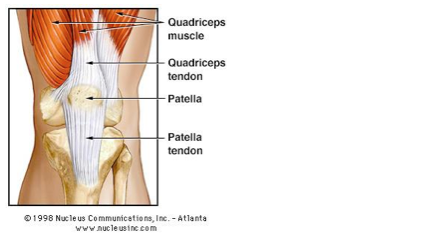
The Patella Tendon
The patella tendon is tendon that is made up of the five quadriceps muscles of the front of the thigh; it starts from above the patella (knee cap), encapsulates the patella, then attaches down onto the tibia (shin bone). The quadriceps muscles’ main function is to extend the knee; this allows effective walking, running, jumping, hopping, stair climbing amongst many others. Therefore the patella tendon’s main function is to transmit the forces created in the quadriceps muscle across the knee and allow the knee to extend with the amount of force required.
Specific Risk Factors for Patella tendinopathy
- Running up and down hills
- Continuous jumping sports (eg basketball)
- Tight quadriceps and hamstrings
- Over-dominant quadriceps strength compared to hamstrings.
- Reduced ankle mobility (for example after an ankle sprain or fracture)
- Poor Biomechanics especially pronation
- Reduced core stability
Symptoms
- Pain when touching the patella tendon
- Pain when running, jumping or coming down stairs; this can be worse with warm up, ease as the movement continues then get significantly worse over the next 24 hours.
- Knee stiffness in the morning
- Reduced “spring” in the legs
- Lack of balance
Physiotherapy Assessment
During a physiotherapy assessment, the therapist may ask a client to walk, run, go up and down stairs, and perform various functional assessments (for example squatting or jumping) to see how the tendinopathy is affecting function and ability. This may be timed or counted and will be used by the physiotherapist to assess how well the client is progressing.
Orthopaedic Investigations
The medical investigation normally used to confirm diagnosis is an ultrasound scan. A consultant may request one to try to diagnose the stage of the condition as this can affect the rehabilitation.
REHABILITATION
This is a general programme that most physiotherapists will use and has been shown clinically to be effective and provide long term management. It is important to note that different physiotherapists may do things slightly differently however the goal is to return the client to their previous level of activity pain-free.
Another important note is that a client may not get 100% improvement from a Patella tendinopathy. The reason for this is that (as explained during the initial article on tendinopathy) some of the processes that cause tendinopathy can involve degeneration of the collagen fibres in the tendon; depending on the amount of this degeneration a tendon’s integrity may not go back to 100%. This is why effective rehabilitation, cross training, strength training and reducing any modifiable risk factors are very important. Nonetheless a physiotherapist will do everything possible to provide a client with a rehabilitation programme to enhance the chance of 100% success and return to sport.
Early Phase Intervention
- Patient education on the condition, and what to do and not to do (e.g. stop squeezing the tendon and no stretching).
- Icing – 15 minutes at a time, every hour if possible.
- Activity modification. This involves avoiding any aggravating activities (e.g. running or jumping).
- Maintaining cardiovascular fitness through cycling and swimming.
- Assess and alter footwear if required; this may include changing trainers or providing orthotics to reduce the foot pronating.
- Quadriceps, hamstring and calf deep soft tissue massage
- Calf and hamstring stretching
- Mid-range leg extensions; this may be on the leg press machine or just in sitting.
- Mid-range lunges
- Single leg calf raises
- Single leg standing to improve balance
- Calf massage, enhanced by using a foam roller or a spikey ball.
- Manual therapy from the physiotherapist to improve any ankle joint stiffness that may be present.
- Addressing core stability with Pilates based exercises or general gym-based exercises (eg TRX movements)
All exercises and activities should be pain-free during the exercise, should not increase pain over the 24 hours after doing the exercise, and should be ceased before fatigue occurs.
To progress to the mid-phase of treatment the client should have reduced pain from the patella tendon, be able to single-leg press 1.5xbody-weight, be pain-free during and for the 24 hours post the exercise.
Mid-Phase of treatment
- Maintaining icing, activity modification and cardiovascular fitness.
- Continuation of Calf massage and manual therapy if needed
- Full range lunges increasing endurance
- Walking lunges no weights
- Split squats; progressing to dynamic split squats (alternating legs), then to jumping split squats,
- Increasing range and repetitions on leg extensions (eg on the leg press machine)
- Increasing repetitions for heal raises
- Continuation of quadriceps, hamstring and calf deep soft tissue massage
- Continuation of hamstring and calf stretching
- Continuation of core stability.
To progress to the end stage of treatment the client should have no pain, be able to single-leg press 1.5xbody weight for 25 repetitions and this is pain-free. A physiotherapist may also choose to ask a client to hop as high as they can or for as far as the can to see how well the Patella tendon is performing.
Late Phase Treatment
- Weighted lunges increasing power (low repetitions, increasing weight)
- Increasing weight and low repetitions for leg press machine
- Machine calf raises increasing weight and reducing repetitions.
- Plyometric training (balancing this with the power work); this can include skipping, hopping.
- Continuation of quadriceps, hamstring and calf deep soft tissue massage
- Continuation of hamstring and calf stretching
- Start quadriceps stretching if painfree
- Continuation of core stability
Return to Sport
- Gradual return to sport using appropriate periodised programme. If this is running, a “return-to-running” programme can be used; this often looks similar to this (days relate to training days):
- Day 1 – walk 20 minutes
- Day 2 – walk 4 minutes, run 1 minute; repeat 4 times to bring to the total time to 20 minutes.
- Day 3 – walk 3 minutes, run 2 minutes; repeat 4 times to bring to the total time to 20 minutes.
- Day 4 – walk 2 minutes, run 3 minutes; repeat 4 times to bring to the total time to 20 minutes.
- Day 5 – walk 1 minute, run 4 minutes; repeat 4 times to bring to the total time to 20 minutes.
- Day 6 – run 20 minutes.
- Day 7 – run 25 minutes.
- Day 8 – run 30 minutes.
- From this point onwards continue to increase run distance by 5 minutes until up to previous length of time run. Once up to a normal time, then reduce back to 20 minutes and increase the pace of the run; gradually increase the time by 5 minutes at this higher pace.
- The entire running programme should be pain-free, and the patella tendon should be monitored throughout the run and for the 24 hours after it. The client must be strict about the timings no matter how good they are feeling; if the tendon is going to flare up, it is unlikely that it will be painful during the run, instead it will be painful over the forthcoming 24 hours. If this happens the rehabilitation programme will have to start from the beginning again.
- Incline running (running up a hill) should be the last thing that is added into any rehabilitation programme.
- Running specific drills; these could include stride throughs, hurdle work, hopping, skipping, bounding.
- Maintain cross training and icing.
- Continue to improvement of core stability.
Conclusion
Hopefully this provides a general programme of what to expect when attending physiotherapy for an Patella tendinopathy. As stated earlier each physiotherapist may do things slightly different and this is purely some guidance.
Any questions that you may have or if you would like further information please do not hesitate to contact the clinic.